Rift valley fever
Rift Valley fever (RVF) is a viral zoonosis that primarily affects animals but also has the capacity to infect humans. It is transmitted by mosquitoes and blood feeding flies. In humans, the disease ranges from a mild flu-like illness to severe haemorrhagic fever that can be lethal. When livestock are infected the disease can cause significant economic losses due to high mortality rates in young animals and waves of abortions in pregnant females.
While some human infections have resulted from the bite of infected mosquitoes, most human infections result from contact with the blood or organs of infected animals. Occupational groups such as herders, farmers, slaughterhouse workers and veterinarians are at higher risk of infection. Humans may also become infected by ingesting the unpasteurized or uncooked milk of infected animals. No human-to-human transmission of RVF has been documented.
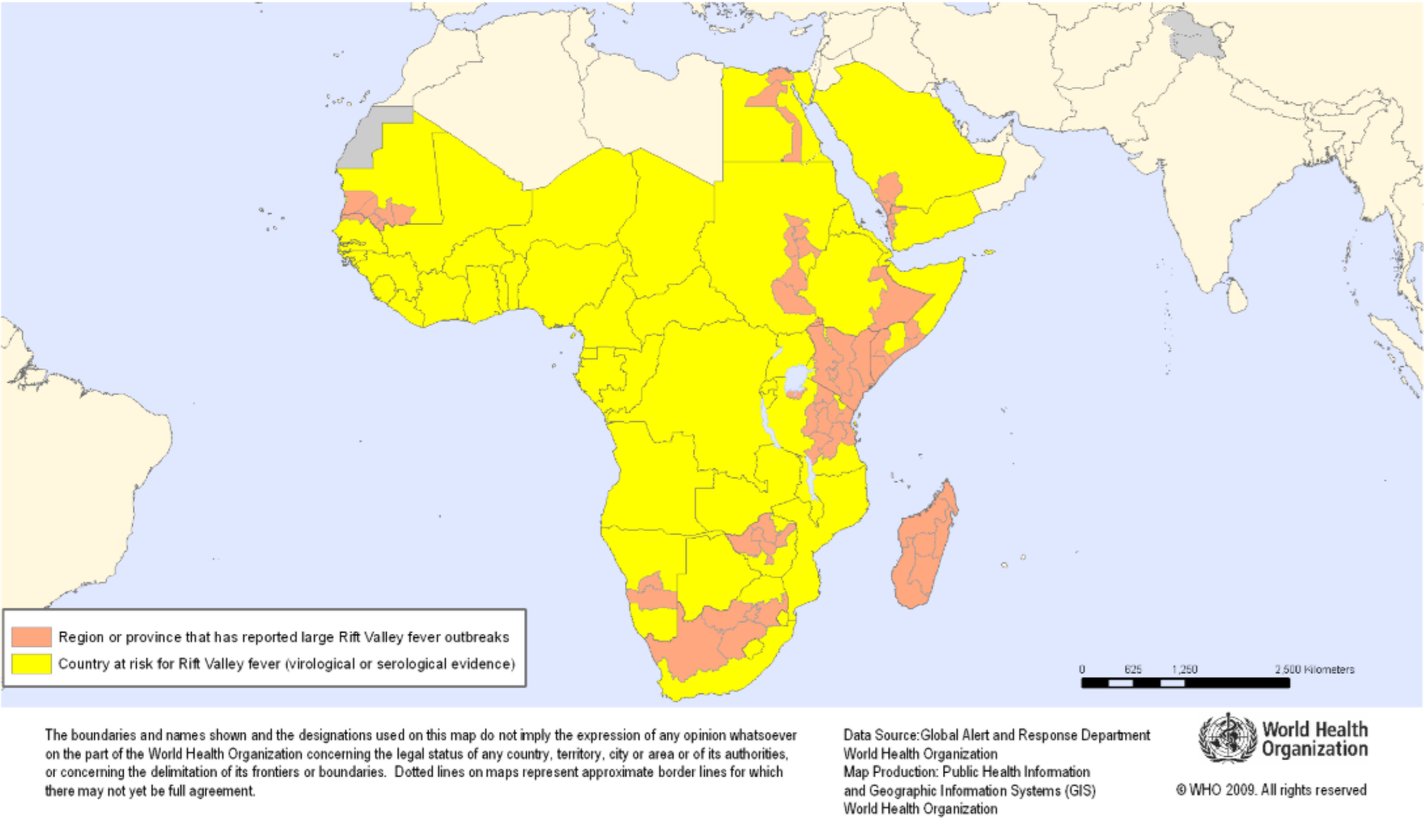
The virus is a member of the Phlebovirus genus and was first identified in 1931 in a sheep epidemic on a farm in the Rift Valley of Kenya. Since then, outbreaks have been reported in sub-Saharan Africa and North Africa. In 2000, the first reported cases of the disease outside the African continent came from Saudi Arabia and Yemen.
Mild form of Rift Valley Fever in humans
The interval from infection to onset of symptoms for Rift Valley fever (RVF) varies from 2 to 6 days. In its mild form, people who are infected with the virus either experience no detectable symptoms at all or develop a mild form of the disease characterized by a feverish syndrome with sudden onset of flu-like fever, muscle pain, joint pain and headache. Some patients develop neck stiffness, sensitivity to light, loss of appetite and vomiting; in these patients the disease, in its early stages, may be mistaken for meningitis. The symptoms of RVF usually last from 4 to 7 days.
Severe form of Rift Valley Fever in humans
While most human cases are relatively mild, a small percentage of patients develop a much more severe form of the disease. This usually appears as one or more of three distinct syndromes: ocular (eye) disease (0.5-2% of patients), meningoencephalitis (less than 1%) or haemorrhagic fever (less than 1%).
The total case fatality rate for RVF has varied widely between documented epidemics but, overall, has been less than 1%. Most fatalities occur in patients who develop the haemorrhagic icterus (jaundice) form of the disease.
Diagnosis
Because the symptoms of Rift Valley fever (RVF) are varied and non-specific, clinical diagnosis is often difficult, especially early in the course of the disease. RVF is difficult to distinguish from other viral haemorrhagic fevers as well as from many other diseases that cause fever, including malaria and typhoid fever. As such, definitive diagnosis requires laboratory testing.
Treatment
As most human cases of RVF are relatively mild and of short duration, patients with this form of the disease require no specific treatment. For the more severe cases, the predominant treatment is general supportive therapy.
An inactivated vaccine has been developed for human use. However, it is not licensed or commercially available. It has been used experimentally to protect veterinary and laboratory personnel at high risk of exposure to RVF. Other candidate vaccines are under investigation.
During an outbreak of RVF, close contact with animals and their body fluids has been identified as the most significant risk factor for RVF virus infection. Risk of animal-to-human transmission of infection can be reduced by avoiding unsafe animal husbandry and slaughtering practices by maintaining good hygiene, and avoiding unsafe consumption of fresh blood, raw milk or animal tissue in affected regions.